By Dee Tomic
It was with a heavy heart that I gave up homemade Nutella sandwiches in third grade of primary school.
The newest member of our class had an anaphylactic peanut allergy, which meant that every afternoon before leaving the classroom for lunchtime, we all lined up while the teacher surveyed our lunch boxes to ensure no nut-related snacks joined us on the playground.
The situation certainly seemed absurd at the time; however, many schools all over Australia have adopted similar strategies to deal with the increasing prevalence of children’s peanut allergies. Today, almost 3 in every 100 Australian children are allergic to peanuts1. Unlike other common food allergies including egg and cow’s milk, peanut allergies tend to persist into adult years, and can often be life long.
As peanut allergy cases rise in Western society, large-scale research studies are being conducted worldwide, investigating the causes, prevention and management of the allergy. Until recently, paediatricians have recommended against exposure to peanuts in early years, particularly for children already affected by health conditions that suggest they may be at risk of developing a peanut allergy. However, a recent study published in the New England Journal of Medicine suggests that early exposure to the nut may actually serve as a protective factor.
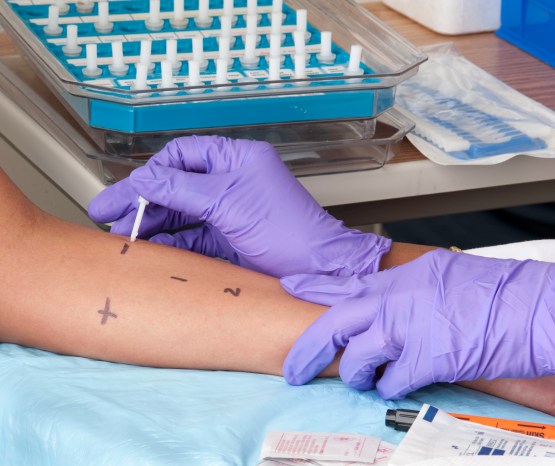
The Learning Early About Peanut Allergy (LEAP) randomised controlled trial was conducted by researchers across the United Kingdom and United States. 640 infants, deemed at high risk due to egg allergy or severe eczema, were randomly assigned to either consume or avoid peanuts until 60 months of age. At the end of the study, a skin-prick test showed that the prevalence of peanut allergy was 35.5% in the avoidance group, and only 10.6% in the consumption group2.
This result has launched food allergies into health news headlines once again.
Further studies are now testing whether the results of the LEAP study can be replicated in the context of other allergies including milk, eggs, sesame and fish.
Researchers for the current Enquiring About Tolerance (EAT) study in Kings College, London, are confident that this will be the case. They observed an increase in children’s food allergies in the UK, whilst consumption of allergenic foods reduced significantly. Yet, for example, in countries across Asia, Africa and the Middle East where children’s diets include peanuts as a staple ingredient, the rate of peanut allergy diagnosis was far lower3. This supports the hypothesis that early introduction of allergenic foods decreases the risk of developing the allergy.
Currently, the trial involves over 1300 infants, and is investigating six allergenic foods by either introducing or excluding them from the children’s diets.
It will be interesting to see the implications of the EAT study results when they are released at the conclusion of the three-year trial. Whether or not there really is a trend between early avoidance and development of allergies, this new research has certainly challenged our current understanding of the immune response.
Another powerful finding from a Swedish study suggests that hand washing dishes, as opposed to using a dishwasher, reduces the likelihood of allergy development. Over 1,000 parents answered questions on asthma, eczema and rhinoconjunctivitis in their children aged seven to eight, as well as about their typical household dishwashing practices.
The study showed that allergic disease development was significantly reduced in children of families who used hand dishwashing (odds ratio 0.57)4. There was a further risk reduction for children who had been exposed to fermented food, and if the family purchased food directly from farms.
These results support an idea commonly known in medicine as the “hygiene hypothesis”. Many scientists believe that increased microbial exposure of children in early years, whether through dirty dishes or farm-fresh foods with high bacterial content, stimulates development of the immune system thus reducing the likelihood of allergies later in life.
Of course, these results do not confirm the hypothesis, and further research must and undoubtedly will be undertaken so we can really gain an understanding of how lifestyle may influence the development of children’s allergic disease.
But with each further investigation, we are a step closer to uncovering the causes of the allergic response, and preventing allergies before their onset.
For three years a friend of mine excluded dairy products from her diet. Recently she tried to re-introduce milk into her regime but found herself unable to bear even a single glass. Her doctor suggested a hydrogen breath test, which much to her surprise, confirmed she had developed lactose intolerance. As she had no previous issues with lactose, or any family history of food intolerances, perhaps her prolonged avoidance of dairy was the turning point.
Could this be the next step for researchers? With diagnosis of food intolerances escalating rapidly, there is a high demand for explanations.
Allergies will certainly be an exciting field of medicine to watch over the coming years. Perhaps soon, we will see new and more effective treatment strategies, and who knows, maybe even the return of Nutella sandwiches to the primary school lunch menu.
References
- Allergy & Anaphylaxis Australia 2015, Peanut, viewed 3 March 2015, https://www.allergyfacts.org.au/living-with-the-risk/allergen-specifics/peanut
- Du Toit, G, Roberts, G, Sayre, P, Bahnson, H, Radulovic, S, Santos, A, Brough, H, Phippard, D, Basting, M, Feeney, M, Turcanu, V, Sever, M, Lorenzo, M, Plaut, M & Lack, G 2015, ‘Randomized Trial of Peanut Consumption in Infants at Risk for Peanut Allergy’, The New England Journal of Medicine, vol. 372, no. 9, pp. 803-813.
- EAT Study 2015, Background, viewed 3 March 2015, http://www.eatstudy.co.uk/background/
- Hesselmar, B, Hicke-Roberts, A & Wennergren, G 2015, ‘Allergy in Children in Hand Versus Machine Dishwashing’, Pediatrics, vol. 135, no. 3, pp. 590-597.

